Let’s be honest — when most people start researching hair transplants, the first question they type isn’t about cost or recovery time. It’s: does it hurt? And honestly, that’s the most human question in the world. Nobody wants to sit in a surgical chair for hours wondering when the pain’s going to kick in.
FUT, or Follicular Unit Transplantation, has a reputation. Some people have heard horror stories — “they cut a strip from your scalp” — and immediately close the browser tab. Others have done the research, talked to surgeons, and walked away thinking it wasn’t half as bad as they expected. So which version is closer to the truth? Well, both, in a way. The honest answer lives somewhere in the middle, and it really does depend on a few things worth understanding before you make any decisions.
Here’s the thing about pain — it’s deeply personal. What one person describes as “pressure” another person might call genuinely uncomfortable. What feels manageable on a good night’s sleep feels brutal when you’re anxious and under-hydrated. So instead of giving you a vague “it’s not that bad” reassurance, let’s actually walk through what happens, stage by stage, so you know what you’re getting into.
What Actually Happens During the Procedure
The FUT procedure begins with local anaesthesia injected into the donor area — that strip of scalp at the back of your head, typically between the ears. And here’s where most patients agree: those initial injections sting. Not in a catastrophic, life-altering way, but in the sharp, unpleasant way that any needle near sensitive skin tends to feel. Some clinics now use a technique called needle-free anaesthesia or a “comfort-in” system, which uses pressure rather than a needle to deliver the local, and patients consistently report that this reduces the sharp bite considerably.
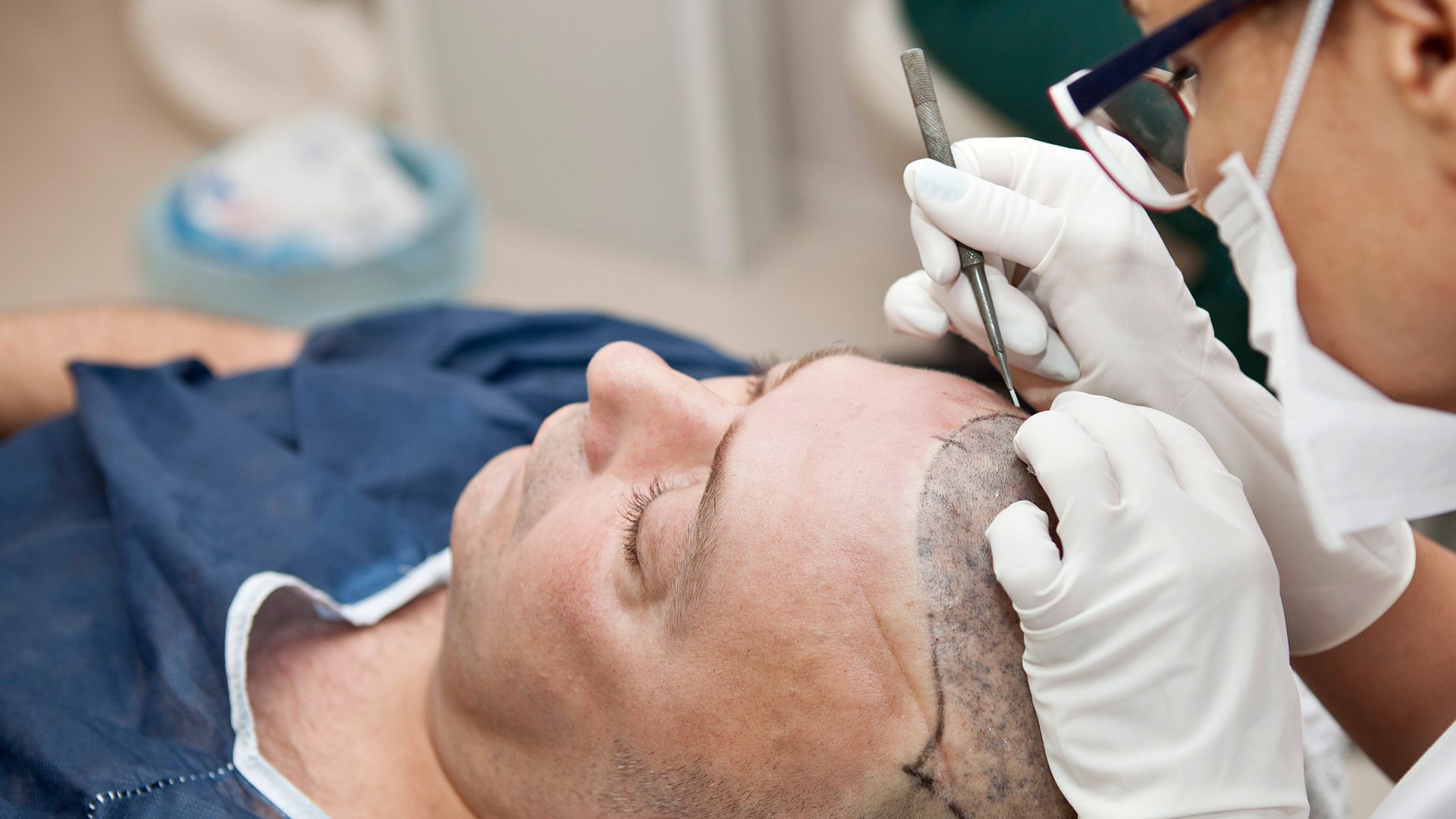
Once the anaesthetic takes hold — which it does within a few minutes — the actual strip excision is largely painless. You’ll feel pressure, movement, tugging. Some people find it deeply weird, that disconnect between knowing something’s happening and not being able to feel pain from it. But weird isn’t the same as painful. The strip of scalp containing the donor follicles is removed, the wound sutured, and then the real time-consuming part begins: dissecting that strip into individual follicular units under a microscope.
This dissection phase is where you’re essentially waiting. The surgical team is working carefully, often for several hours, preparing hundreds or even thousands of grafts. Meanwhile, the recipient area — where follicles will be implanted — also needs anaesthesia. More injections, more stinging, same story. After that? The implantation itself is typically described as nothing more than mild pressure. You’re numb, you’re lying down, and honestly, most patients say they dozed off at some point.
The procedure can run anywhere from four to eight hours depending on the graft count. That’s a long time to be reclined in a chair, and fatigue definitely sets in. But pain during the actual surgery? For most people, once the anaesthetic is working, it’s not the word they’d use.
The First Few Days After Surgery
Post-operative discomfort is where FUT distinguishes itself from its sibling procedure, FUE (Follicular Unit Extraction). Because FUT involves removing a linear strip of tissue, there’s a sutured wound at the back of the head that needs to heal. And that suture line? For the first two to five days, it can be genuinely sore.
Patients commonly describe a tight, throbbing sensation across the donor site. Sleeping becomes a bit of a puzzle — you need to keep your head elevated, usually at a 45-degree angle, to minimise swelling. Most surgeons prescribe a short course of pain relief (typically something like ibuprofen or a mild prescription analgesic), and the majority of patients find this keeps things manageable. “Uncomfortable” rather than “agonising” seems to be the consensus.
Swelling is another factor people don’t always anticipate. It tends to peak around days two to four and can migrate down toward the forehead and eyes. It looks alarming. It’s rarely as painful as it looks, but it does add to the general sense of soreness and heaviness. Cold compresses help, and most swelling resolves within a week.
The recipient area — where the grafts were placed — tends to feel tender rather than painful. There’s often itching as the scalp begins to heal, which can be maddening in its own right but isn’t exactly pain. Scratching is off-limits for obvious reasons, so you’re left with the mild frustration of an itch you can’t address. Some clinics recommend saline sprays to keep the area moist and reduce that irritating sensation.
By day five or six, most patients feel significantly better. The sutures typically come out around day ten to fourteen, and that removal process — contrary to what you might fear — is usually painless.
FUT vs. FUE: Is One Actually Less Painful?
This comparison comes up constantly, and it deserves a clear-eyed look rather than a marketing answer. FUE has been increasingly positioned as the “less painful” option, and there’s truth in that — but it’s more nuanced than the brochures let on.
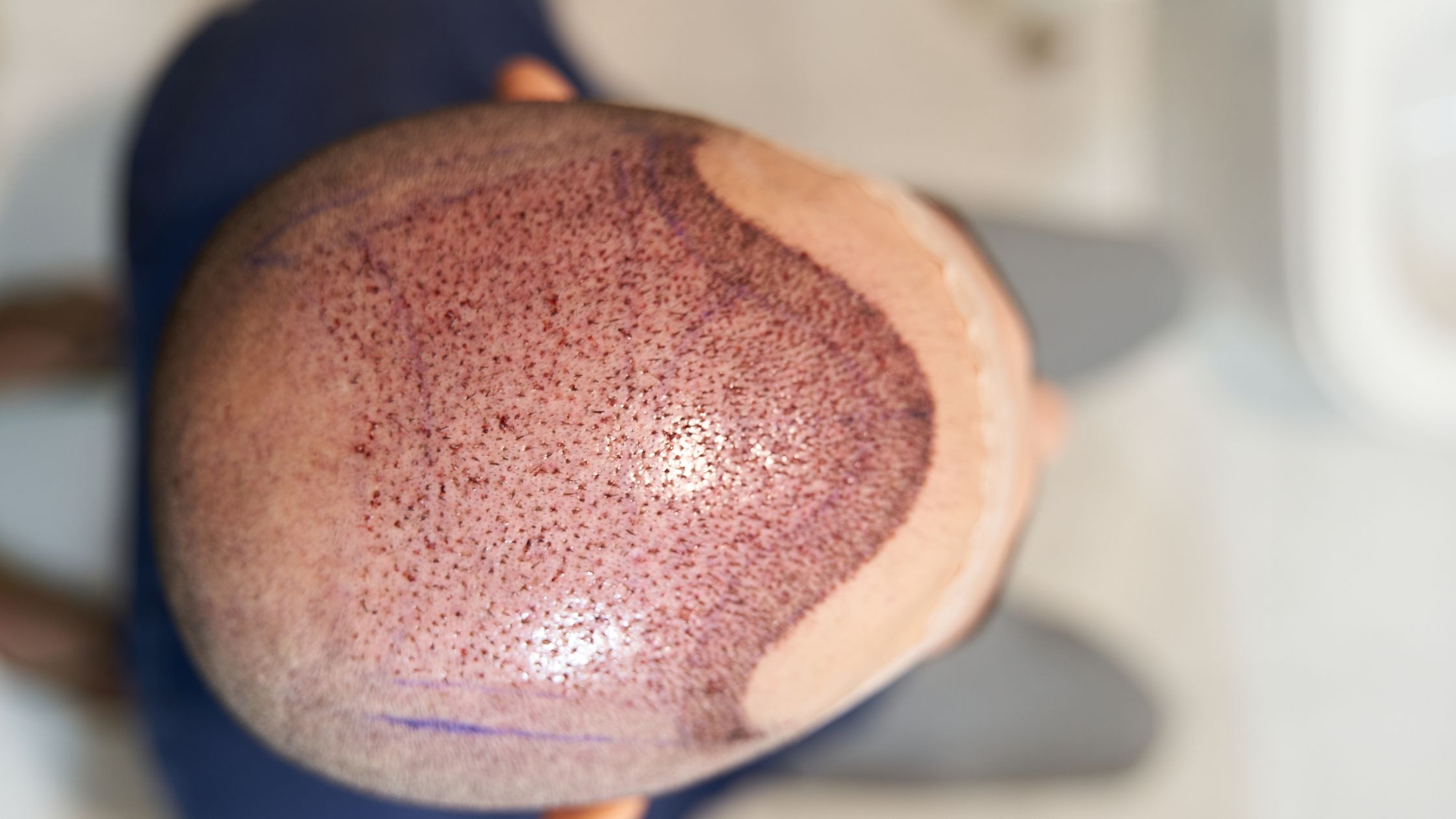
FUE doesn’t involve a linear incision or a suture line, so you’re not dealing with that specific kind of post-op soreness. The donor area in FUE looks like a scattered series of tiny punch wounds rather than a single strip. That generally means less acute pain in the first days after surgery. Recovery is often described as faster, and many patients return to desk work within two or three days.
But — and this is worth knowing — FUE has its own discomforts. The punching of individual follicles can take longer and involve more anaesthetic injections across a wider area. Some patients experience more widespread tenderness across the entire donor zone rather than concentrated soreness at a single suture site. The difference in pain profile is real; which one is “better” honestly depends on your personal tolerance and how your body responds.
FUT, despite its more invasive-sounding description, has one thing going for it: it often delivers more grafts in a single session, which matters if you have significant hair loss to address. Surgeons who specialise in the technique — and there are still many who prefer it for certain patients — argue that the linear scar, when placed correctly, is undetectable under a short haircut and that the pain-to-outcome ratio is entirely reasonable.
What both procedures share is a roughly similar experience during surgery itself — local anaesthesia, minimal pain once numb, mostly pressure and waiting. The real divergence is in those first post-op days and in the nature of the scarring. For anyone considering which route to take, a consultation with a board-certified surgeon who performs both is worth more than any online comparison.
How to Make It Easier on Yourself: What Actually Helps with Pain Management
You know what makes pain worse almost universally? Anxiety. Going into a procedure tense, sleep-deprived, and half-convinced something will go wrong is a reliable way to amplify every sensation. The patients who consistently report the best experiences are those who walked in informed and relatively calm — not because they’re unusually stoic, but because they knew what was coming and therefore weren’t frightened by normal sensations.
There are a few practical things that genuinely help. First: follow your surgeon’s pre-operative instructions. Avoiding alcohol for at least a week before surgery, stopping blood-thinning supplements like fish oil or high-dose vitamin E, and getting a proper night’s sleep the night before all make a measurable difference to how your body handles the procedure.
During the procedure, distraction is your best friend. Most clinics now have screens where you can watch films or series; many patients put headphones in and listen to podcasts or music. A long Netflix session has gotten more than a few people through what might otherwise feel interminable. Bring something absorbing.
Post-operatively, take the medication your surgeon recommends — don’t try to tough it out unnecessarily. Sleep elevated. Apply saline mist as directed. Avoid anything that raises your blood pressure significantly for the first week (so: intense exercise, hot baths, spicy food in excess). These aren’t arbitrary rules; they directly affect swelling and healing speed.
One thing that’s easy to overlook is the psychological side of recovery. “Shock loss” — where transplanted and surrounding hairs fall out in the weeks after surgery before regrowth begins — can be alarming if you’re not expecting it. It’s a normal part of the process, but coming across it without warning can spike anxiety and make the recovery feel harder than it actually is. Ask your surgeon about it in advance.
The full results of a FUT transplant typically become visible somewhere between nine months and a year after surgery. Some people start seeing growth as early as three to four months; others wait longer. Either way, the pain — such as it is — is long behind you by the time the results start showing up. And for most people, that’s a trade-off that ends up feeling entirely worth it.
So — is a FUT hair transplant painful? The straightforward answer: the surgery itself, with modern local anaesthesia, is overwhelmingly described as pressure and discomfort rather than pain. The first few post-operative days can be sore, especially around the suture line. Most people manage it comfortably with standard pain relief and find that by the end of the first week, they’re feeling pretty normal again. It’s not a walk in the park, but it’s also not the ordeal some people fear it to be.
What matters most is choosing an experienced surgeon, going in prepared, and giving your body the space to recover properly. The pain, where it exists, is temporary. The hair, done well, is not.